Three weeks ago I had open heart surgery to replace a failing bicuspid aortic valve with an On-X mechanical valve. I’d say that I’ve bounced back extremely quickly, but one little-discussed consequence of surgery like this is the emotional effects- anxiety, depression, doubt. I am writing this in case you’re interested, but mostly so I can get my thoughts and feelings out. I’ll get back to coding stuffs in future posts 🙂
A history of vague sickness…
I’m 32 and I’ve been a runner since I was 10. Every visit to the doctor was unremarkable until I was in my mid twenties. Suddenly, after returning from my fourth trip to Hong Kong and China I was struck with severe flu symptoms. The next two years I battled through what doctors would call fibromyalgia.
Fibromyalgia is debilitating because you hurt everywhere and you’re tired but there’s seemingly no reason for it. I found through many diets, doctors, and books that the best way to improve was through exercise. I began a running program where I started with an embarrassing 5 minutes of running and then did that every other day, slowly increasing running times by a minute about a week. After a few months I was back to running 30-45 minutes consistently, and my symptoms improved. I felt like I was at 80%.
I never did fully recover, though. I was tired all the time despite feeling better. I couldn’t sleep well. I noticed through my Fitbit that my heart rate was high, even while resting, and the doctors started to noticed that my blood pressure was starting to inch up. It was regularly 125/60. Higher systolic blood pressure was weird, and the doctors had no explanation for me, so we didn’t do any medications to control it.
I had suspicions that there might be something heart related going on. I always knew that my heart rate was higher than most, and I found it strange that I could see my heart rate in my chest when I was at rest (my chest would move with every heart beat), but until this point 2017 doctors were avoiding a stress test or any kind of echocardiogram.
Anxiety, breathlessness, and doctors
In 2018 I was starting to get chest pains. I had moments where I couldn’t breath very well, even when I was just at my keyboard or watching tv. I went to the emergency room on three separate times because I was out of breath, and I went back to my doctor. I was noticeably short of breath on my regular runs. Sometimes when I went on walks with my friends or family I needed to ask them to slow down. My heart rate was now around 140/70 at rest.
My doctor suggested I was dealing with panic attacks, and prescribed a fibromyalgia/anxiety medication called Cymbalta. He also gave me Lorazepam to help me when I had “panic attacks.” Still, life was starting to get unmanageable because I couldn’t exercise, and when I was short of breath I had a really difficult time focusing on work and family.
Looking back, I know that anxiety wasn’t the primary issue. I had anxiety at times because I couldn’t breath. It’s a chicken or the egg scenario, and I think my doctors guessed wrong. Anxiety can cause breathlessness, but I think my breathlessness caused me the most anxiety. I often wonder where the communication broke down. I have to push aside resentment over my previous doctors not investigating further because they are mere mortals and did the best they could. Forgiveness is following the golden rule, but resentment kills the soul.
What led me to heart surgery
In August of 2018 I pushed my doctor more to get a stress echocardiogram. He didn’t think I needed it, but I said I wanted to do it anyway to make sure. So after pedaling on a bike for about a half an hour and having an ultrasound of my heart, I found out that I had a congenital heart disease called bicuspid aortic valve.
At the time my regurgitation was classified as “low to moderate.” This meant that a low to moderate amount of blood slid back into my heart once a heart beat finished. This was fairly normal for people with BAV, and many people who have BAV (about 1-2% of the population) have no idea anything is different until they feel short of breath in their 60s or 70s.
The cardiologist I saw afterwards said that I was “very low risk,” and I probably would need surgery, but it would be 15 years or so in the future. All the doctors I had at this time were fairly certain that my recent symptoms were not cardiac in origin. This was hard for me to accept, but I tried to move on.
Around November of 2018 I had a number of different people suggest I apply to go to Mayo Clinic to get a second opinion. I did just that, and had a slew of appointments scheduled in December. After about 7 days of non-stop tests and consults, it was confirmed that fibromyalgia was a likely explanation for what I was experiencing. But, I had one consult remaining on December 26th with the cardiologist.
I remember going to the cardiologist and expecting nothing different to happen- everything so far seemed to suggest I was still just struggling with fibro and nothing more.
I was shocked to hear the cardiologist when he looked at the same images that were taken a few months before and classified my regurgitation as “quite severe.” Apparently my valve opened in a “strange” way. He said that I needed another echocardiogram to take some more measurements, but surgery was very likely.
The emotions from that meeting were mixed. I felt relief knowing that there may be some vindication for feeling so awful for for so long and not having answers, and that anxiety wasn’t my main issue. There was also some sadness because this meant heart surgery.
After another echo my new cardiologist called me back and confirmed that surgery was a probably next step. My heart was getting larger, probably due to the strain of a leaky valve. He said that I was right at the cusp of needing the surgery, but I could wait if I really wanted to. I did not want to wait
Preparing for heart surgery
I was referred to a specialist who only worked with mitral and aortic valves at Mayo, and she guessed that I would need surgery in the next year or two. She confirmed a bunch of symptoms and phenomena that happen with a failing aortic valve. She recommended a mechanical valve since a biological replacement or a correction would probably wear out very quickly.
Since I would probably need it anyway, and I was feeling pretty miserable, we went ahead with surgery.
We had consults with my wonderful surgeon and his team. I learned a lot about what to expect, about Warfarin (Coumadin) and blood thinners, and about the different type of valve corrections and replacements. I was keeping busy at work, but it felt like my life was put on hold until this resolved.
At times I was anxious about having to wait 2 months for surgery. I was anxious about the chest pains I felt, and at times very anxious about the outcomes and dangers of surgery. But I made it.
Heart surgery
I got a dental checkup. Most people don’t know that oral health is strongly related to heart health. I didn’t. I also washed with a special antibacterial soap. We checked into Mayo on March 18th and they prepped me. Every time I went to a new room they asked me for my name, birthdate, and what the procedure would be.
I was fortunate to have a surgeon that could do “minimally invasive” surgery, which means instead of open heart he could replace the valve through a smaller incision and by removing one of my ribs. He said the worst case scenario is that he might have to do an open heart surgery if there were complications.
When I woke up they informed me that that’s exactly what happened. Most of the way through the surgery there were issues in locating certain arteries, and they had to open my chest by sternotomy.
The valve was replaced just fine, though, and things were apparently looking good. Now it was time to go to ICU and recover.
Recovery
Most people say full recovery can take 3-6 months or longer, and I’m currently at one month. The first week was by far the worst part.
After the ICU was eventually moved to what’s called a step-down unit. There, I tried to regain some of the bodily function I lost when I was anesthetized: constipation, inability to relieve yourself, shallow breath, and pain were all huge issues for me.
Pain relievers had side effects or didn’t work for two days for me, and until they found the right pain reliever I was struggling along with Tylenol. I tried to go for walks, but the process was extremely tiring, and you have to use a walker. Most people don’t know that you have tubes left over from surgery and pacemaker leads still inside you for about 3-4 days to make sure you don’t retain fluids and your heart beat remains consistent. Every movement was awkward with all these tubes and wires, and I felt like my old self was gone.
Eventually, with tubes out and the proper pain relievers, I felt good enough to go home.
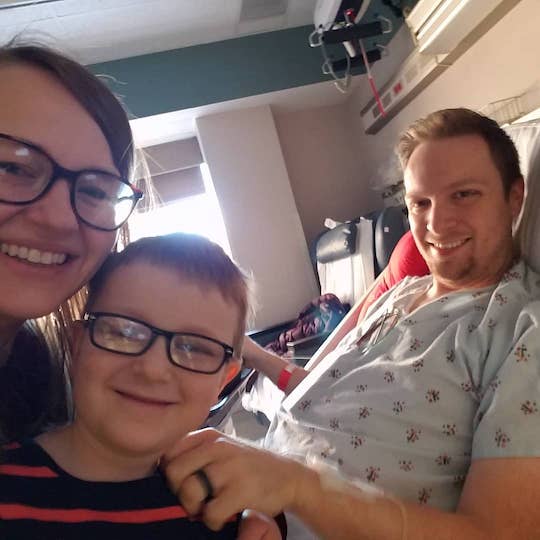
My wife and oldest at the hospital 
My wife and second oldest
After that first week recovery seemed to speed up every day. I’m feeling close to normal now, but I have restrictions: not lifting anything heavier than 10 pounds, not exercising past a certain point, going to physical therapy, not driving…
The real battle has been emotional and mental lately. There are a lot of risks now with blood thinners and my valve. Did I do the right thing? Will I have to worry about blood clots? Will my blood pressure return to normal? Will my ejection fraction recover?
My goals now are to get back to running and rock climbing and to be able to pick up my four kids. Luckily I work in an field that requires a lot of brain power and not physical power- I’ve been able to do so much and learn so much in coding and tinkering with aruinos/raspberry pis at home during this period.
Life keeps going, and I’m thankful that we were able to catch this, and in the words of the person doing my echocardiogram, “You have a beautiful valve protecting your heart.”
That’s all for now
That’s about it right now. There is some anxiety that I’m still working through now. Ultimately, I believe God intends all things for a purpose, and that he’s in control. One day at a time.
If you’ve read this far, thanks! I hope it’s encouraging or edifying. I’d love to hear your thoughts. Feel free to comment or tweet me at @jschof.
So lovely to hear your journey……many people will benefit from these words. At such a young age one never thinks they will be dealing with this…….thanks for sharing your unique circumstances, as education is the path to evolution. You are a very brave soul………
Praying for your recovery. My dad had open heart surgery twice when I was a young, and I remember his struggle to recovery and his pain from laughing or coughing. Thanks for sharing this. I hope you get well soon.
You’re a rockstar! So glad you made this decision, it was the right choice.
Hey Jim!
Just read your journey. Incredible man, glad you are on the uptick. Praying for you and your family. Glad you kept in pursuit of answers. I don’t think I was ever able to ask you a question about math that you could not answer! 🙂 Have enjoyed picking through your gutenburg blocks as well.
Regards,
Jim, Thank you so much for sharing. I have a brother who works in the medical field makeing catheders and valves so I sometimes hear about the medical side but not the emotions that go along with it. Thanks for putting it all together. So glad you are on the mend.
Jim, that was a wonderful story. I’m sorry you had to go through all of that. I’m thankful you went to Mayo. My takeaway from this [and my experience suffering at the hands of doctors], is GO STRAIGHT TO MAYO. I love the team approach there. I will pray for your continuing recovery and good health in the future. You’re a good writer.
Jim, I love ya buddy. I’m glad to see your smiling face again, I missed ya. If you need anything, just let me know.